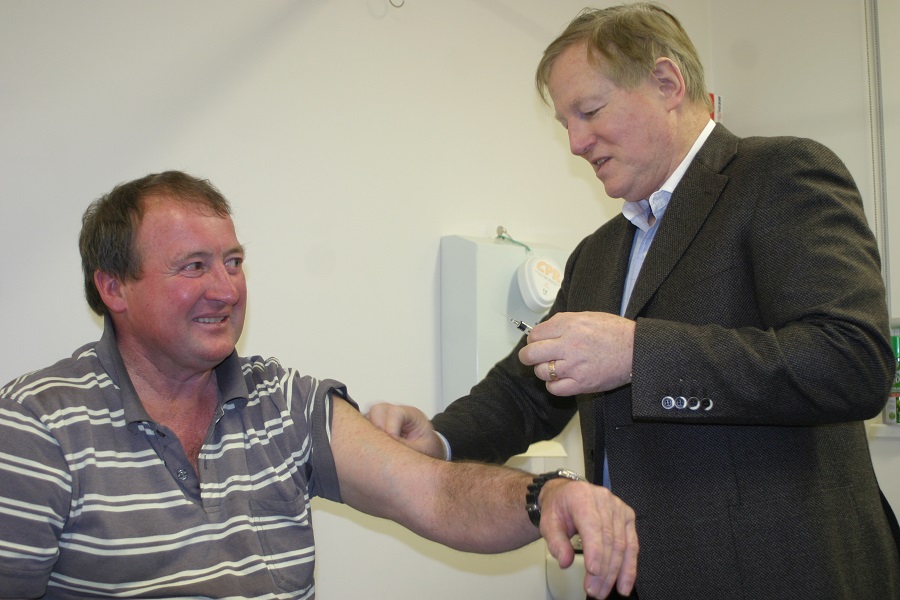
Hamilton’s Dr Dale Ford gives Casterton livestock carrier Mick Smith his Q Fever vaccination in 2015.
GREATER awareness about Q Fever diagnosis among veterinarians and human health professionals was needed, national surveys have indicated.
The surveys by Charles Sturt University have found that only 50 percent of diagnoses among respondents were made by general medical practitioners.
Many people reported that the time to diagnosis was months to years and the path to diagnosis was often identified as not being straightforward. Severe long-term illness and debilitation was reported amongst patients.
The university researchers believe a simple question like “Could it be Q Fever?” could improve patient outcomes and Australia’s ability to limit the likelihood of a prolonged outbreak of this infectious disease.
Q Fever can move from animals to humans and while many people do not become sick or only suffer a mild illness, for others the impact can be long-lasting and debilitating.
New results from Charles Sturt University surveys as part of a national project, ‘Taking the “Query” out of Q Fever’ has shown the need for greater awareness amongst veterinarians and health professionals.
Charles Sturt Associate Professor Jane Heller said a survey of more than 100 veterinarians found gaps in knowledge and confidence in diagnosing the disease in animals.
“The bacteria Coxiella burnetii causes Q Fever in people and coxiellosis in animals.
“Given the limited effect on animals, only one of the vets surveyed had diagnosed coxiellosis and the majority of respondents didn’t feel confident in detecting or recognising the clinical signs of the disease,” Professor Heller said.
But she said more than 68pc of the vets surveyed thought coxiellosis is an important disease of animals.
“The vets surveyed identified the potential for production impacts, the risk of an outbreak and the transfer of infection from animals to people as key issues.
“The majority also felt that vets and General Practitioners (GPs) have a mutual responsibility to report Q Fever,” Professor Heller said.
Professor Heller’s research team included Charles Sturt PhD student Dr Tabita Tan, research assistant Lynne Hayes, and Bachelor of Veterinary Science/Bachelor of Veterinary Biology Honours research student Dr Jesse Fox.
Further research also examined the experiences of people who’ve had Q Fever.
Professor Heller said around 200 people took part in an online survey, with 14 in-depth interviews conducted by Charles Sturt researchers.
“The survey showed that some patients experienced severe, long-term illness and debilitation.
“A number of people said it took months or even years to be diagnosed with the disease and more than half also found the path to diagnosis was not straightforward,” Professor Heller said.
Professor Heller said this is significant, because Australia has one of the highest rates of Q Fever in people in the world and early diagnosis can improve patient outcomes.
“Acute Q Fever can be treated with antibiotics but it can be difficult to diagnose because patients often present with non-specific clinical ‘flu-like’ symptoms.”
Professor Heller said the research also found that diagnosis of Q Fever was often influenced by the diagnosis of others,” she said.
“The survey found that 28pc of respondents were part of a Q Fever cluster with more than half of those people identifying that their diagnosis was influenced by the diagnosis of others.
“What we were hearing was that people were prompted to ask their healthcare professionals about Q Fever because they had heard about other people with similar symptoms being diagnosed with the disease.”
Professor Heller said this highlighted the need for more awareness about the disease.
“Q Fever is often associated with people working in abattoirs, but the disease can affect many other groups in the population.
“Sheep, goats and cattle are most often thought to be the source of human infection in Australia and intensive management of these livestock can lead to ongoing spread of Q fever,” she said.
“Wildlife, dogs and cats have also been associated with human cases and outbreaks and the bacteria shed by infected animals can survive for a long time leading to people becoming infected through environmental contamination.”
Professor Heller said it’s important that people understand more about the disease and the potentially serious impact on human health.
“We hope that this research will prompt vets, GPs and those people at most risk to ask questions about Q Fever,” she said.
“Vaccination is the best prevention strategy we have for reducing risk of outbreaks, and the human vaccine has been used in Australia since 1989 and has shown to be very effective at reducing the rates of Q Fever.”
Information gathered from the surveys has informed the development of guidelines for an emergency response plan to prevent or limit the impact of a large Q Fever outbreak in humans in Australia.
“The research has highlighted the opportunities to create better communication structures between animal and human health professionals when it comes to Q Fever.
“We believe a multi-disciplinary approach would be important if we were to see a large Q Fever outbreak in the future,” Professor Heller said.
The ‘Taking the “Query” out of Q Fever’ project has been supported by funding from the Australian Government Department of Agriculture, Water and the Environment as part of its Rural Research and Development for Profit program (RnD4Profit-15-02-008), through AgriFutures Australia (Rural Industries Research Development Corporation).
It includes animal health and infectious disease experts from the University of Melbourne, University of Adelaide, the University of Queensland, Charles Sturt University, the Australian Rickettsial Reference Laboratory, Goat Vet Oz and Meredith Dairy.

HAVE YOUR SAY